In the face of economic pressure, rising claims complexity, and a shrinking healthcare workforce, many workers’ compensation programs are revisiting cost containment strategies. One area often scrutinized is nurse case management (NCM), where the appeal of lower hourly rates or contractor-based models can seem like a logical savings move.
But low-cost case management often reveals itself to be a high-cost decision—even if it shows up somewhere other than the NCM invoice.
The Illusion of Savings
At a glance, cutting NCM costs by selecting the lowest-rate provider appears efficient. But when measured across the lifecycle of a claim, price-based decisions can generate unintended and often unseen consequences. In practice, “cheaper” case management tends to mean:
- Delays in initial contact with the injured worker
- Limited oversight and inconsistent follow-through
- Inability to respond swiftly to time-sensitive (Rush) assignments
- Less engagement with the nuances of the claim, including co-morbidities or pre-existing risk factors
- Financial incentive to keep the claim open longer or not handle the claim as proactively
- Less engaged NCMs since lower cost providers often use contractors who are not employees and don’t have ties to the company culture in the same way employees do
Each of these issues can result in extended claim durations, increased treatment delays, higher indemnity costs, and greater exposure to litigation. Read more about The Illusion of Savings.
The Role of Quality in Claim Outcomes
A growing body of research supports what claims leaders know intuitively: early, consistent, and clinically sound intervention is a major driver of total claim cost reduction. Nurse case managers who can quickly engage with all stakeholders, identify barriers to recovery, and coordinate effective care have a direct influence on both the human and financial outcomes of a claim.
Unfortunately, those attributes are not guaranteed in all case management models, particularly those that rely heavily on decentralized contractor panels or prioritize volume over outcomes.
Shifting from Time-Based to Outcome-Based Thinking
One core challenge in evaluating NCM is that many systems still focus on time spent rather than progress made. A nurse logging minimal hours may appear efficient, but if they fail to move the case forward, the downstream costs—delayed return to work, prolonged disability, unnecessary treatment—are substantial.
Organizations are increasingly looking for ways to better align case management metrics with actual claim progress. This includes evaluating not just hours worked, but:
- Milestones achieved
- Medical and work status advancement
- Timely referrals and follow-ups
- Overall claim duration reduction
Shifting to an outcomes-oriented mindset can help employers and payers make more strategic decisions about their vendor partnerships.
Price Should Not Be the Primary Metric
In today’s environment—marked by provider shortages, aging workforces, and rising co-morbidity rates—claims are getting more complex, not less. Case management must evolve accordingly.
The real cost of case management isn’t measured at the invoice level. It’s measured in the ripple effects of missed opportunities, delayed interventions, and under-managed claims.
Executives and claims leaders would do well to remember: the cheapest option up front is often the most expensive over time.
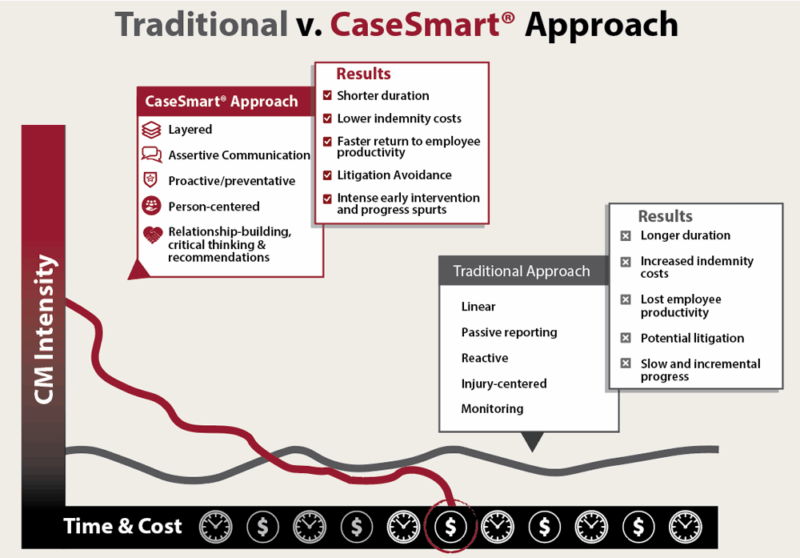
Why ISYS Case Management?
ISYS Solutions was built on the belief that nurse case management should be measured by clinical impact, not just time. Our CaseSmart® approach uses full-time, locally based nurse case managers to respond with urgency, manage with consistency, and move cases forward with purpose. From Rush assignments to complex comorbidities, we deliver results that reduce claim duration and support real recovery, for the injured worker and your bottom line.



No responses yet